Healthcare & Fitness ,
Fitness app exclusively for women
Our esteemed client from Abu Dhabi wanted us to build an app for their Health & Fitness service. This service is exclusively for women. Our develop...
Peerbits deploys purpose-built AI agents that autonomously manage your entire prior authorization lifecycle — detecting requirements, assembling clinical evidence, submitting to payers, tracking status, and appealing denials — without a single phone call from your staff.
Standards & Compliance
Traditional PA tools submit forms. Peerbits deploys AI agents that reason about payer criteria, make decisions, and take actions — the same way a specialist would, but at machine speed. 24/7.
Old Way vs. AI Agent Way
Submission
Staff opens payer portal, copies data, uploads documents, calls for status.
Agent detects PA need, pulls docs from EHR, submits via API, monitors autonomously.
Denial Handling
Denial received — staff manually drafts appeal letter, re-submits days later.
Denial triggers agent — AI reads denial reason, generates appeal, re-submits in minutes.
Pre-Check
Criteria mismatch causes rejection — staff calls payer, reworks documentation.
Agent pre-checks criteria, identifies documentation gaps, requests CDI clarification before submission.
PA AI Agent is a purpose-built AI system that can independently perceive clinical context, reason against payer medical policies, plan a submission strategy, execute multi-step actions across payer APIs, and adapt when it encounters denials — all without waiting for a human to initiate the next step.
Unlike rule-based RPA bots that break when a payer portal changes a button, our agents are AI-enabled with natural language understanding — they read policies, interpret clinical notes, and handle exceptions intelligently. Humans stay in the loop only for complex escalations that genuinely require clinical judgment.
The result: your PA team shifts from executing authorizations to overseeing an AI workforce that handles 91% of cases autonomously.
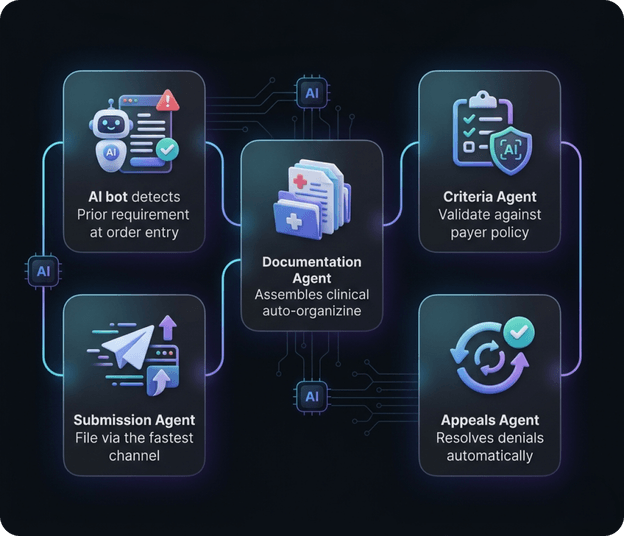
Each agent is purpose-trained for a specific task in the PA lifecycle — working together as an autonomous team that owns the entire workflow end to end.
Monitors every order in real time. Automatically identifies which procedures, drugs, and services require prior authorization based on the patient's specific plan and benefits — before scheduling.
Reads clinical notes, lab results, imaging reports, and medication history from the EHR using NLP. Assembles the exact documentation package each payer requires — nothing missing, nothing redundant.
Reads and interprets each payer's active medical policy documents in natural language. Cross-references patient clinical data against coverage criteria and flags gaps before submission to prevent preventable denials.
Selects the fastest available submission channel per payer — API, EDI 278, or intelligent portal automation — and executes the submission autonomously. Monitors acknowledgement and routes exceptions.
Polls payer systems continuously for status updates. Automatically escalates requests nearing care dates, flags pending peer-to-peers, and notifies clinical staff only when human judgment is needed.
When a denial is received, the agent reads the denial reason, diagnoses the root cause, and autonomously generates a clinically accurate reconsideration letter — with supporting evidence — within minutes.
From order entry to final disposition — every step is owned by an AI agent, with human oversight exactly where it belongs.
STEP 1
The Detection Agent intercepts orders in the EHR the moment they're placed, checks real-time benefits and payer rules, and instantly classifies urgency without any staff action.
STEP 2
Using clinical NLP, the agent reads the EHR — notes, labs, imaging, history — and builds a complete, payer-formatted documentation package. CDI gaps are flagged for clinician review.
STEP 3
The AI reads the payer's medical policy in plain language, cross-matches patient data to coverage criteria, and pre-empts denial triggers — before a single byte is sent to the payer.
STEP 4
The agent selects API, EDI 278, or portal automation based on payer capability and submits the completed PA autonomously — with full audit trail and acknowledgement tracking.
STEP 5
Denials trigger the Appeals Agent immediately — it reads the denial reason, generates a targeted reconsideration letter with clinical rationale, and re-submits — often before staff even see the denial.
Our agents are configured for your specialty workflows, payer mix, and EHR environment — not a generic PA portal that treats all requests the same.
Enterprise agent deployment across inpatient admissions, surgical scheduling, oncology, and imaging — integrated with case management and utilization review workflows.
High-urgency drug authorization agents for chemotherapy, biologics, and specialty infusions — with AI-powered step therapy override and peer-to-peer support.
Pre-surgical authorization agents that auto-pull operative notes, imaging, and clinical history from the EHR and match them against payer criteria for joint replacements and spinal procedures.
AI-enabled continued stay authorization agents with parity compliance checks, level-of-care justification generation, and automated LOS extension management.
High-volume imaging PA agents with built-in AIM/eviCore guideline matching at order entry — eliminating scan delays and reducing radiology PA staff workload by over 80%.
AI-enabled Medicare and Medicaid PA agents for home health admissions, DME authorization, and HHCAHPS-compliant documentation — with ADR response automation built in.
Every feature is agent-driven or AI-enabled — not rules-based automation that breaks when exceptions arise.
The Detection Agent queries payer benefits APIs at order entry — instantly knowing whether PA is needed, what criteria apply, and how urgent the timeline is.
AI reads clinical notes and generates payer-specific medical necessity narratives aligned to each payer's coverage policy — written in the language that gets approved.
The Criteria Agent interprets payer medical policies using LLM reasoning — not keyword rules — and identifies the exact documentation needed to satisfy coverage requirements before submission.
Agents poll payer systems continuously — no manual status calls. Smart escalation alerts surface only the cases that need a human, with full context already assembled.
The Appeals Agent reads denial reasons, diagnoses the root cause, drafts a targeted reconsideration letter with clinical evidence, and re-submits — often before the clinical team is notified.
Real-time dashboard tracking agent approval rates, zero-touch rates, denial reasons, and turnaround times by payer, specialty, and procedure — with actionable AI recommendations.
Identify how our experts solved business challenges leveraging technology by reading case studies.
Legacy PA tools automate steps. Peerbits agents reason, decide, and act — handling exceptions intelligently, not failing silently when something doesn't match a rule.
RPA bots follow scripts and break on exceptions. Our AI agents understand context, read policy language, and handle edge cases the way a trained specialist would — without needing every scenario pre-programmed.
We don't deploy generic agents. We configure each agent for your EHR, your payer mix, your specialty workflows, and your documentation patterns — tailored from day one.
Our agents connect natively to Epic, Cerner, Meditech, and 25+ platforms. They read clinical documentation directly — no copy-paste, no dual-entry, no missed attachments.
Agents handle 91% of cases autonomously. For the 9% that need clinical judgment — complex exceptions, peer-to-peers, ethical considerations — agents route to humans with full context ready.
Unlike SaaS PA platforms charging per transaction, Peerbits builds and delivers AI agents you own outright. As PA volume grows, your cost-per-auth drops — not climbs.
Agents are built on HL7 FHIR R4 and Da Vinci implementation guides — fully aligned with the CMS Prior Authorization Rule (CMS-0057) and ready for mandatory FHIR PA interoperability.
Generic PA platforms give you a portal and a per-transaction bill. Peerbits deploys six purpose-built AI agents — integrated into your EHR, trained on your payer mix, reasoning against actual medical policies — that own the entire PA lifecycle from detection through appeal resolution, at a fixed cost you control.
Benchmarked across 130+ agentic PA deployments against pre-automation baselines.
94%
Agent first-submission approval rate
Manual avg: 71%
91%
Zero-touch authorization rate
No staff involvement required
5.2 hrs
Average agent approval TAT
Manual avg: 2.3 days
$3.8M
Annual admin savings per health system
Per 500-bed deployment
#clientspeak
Learn more about our processes from our clients
After a rigorous selection process choosing Peerbits as our technology partner was the right choice. Peerbits is an innovative company with a team of talented, committed, and smart individuals. Thank you for helping us deliver world-class healthcare solutions. Good job.
Health vector
Start with a free PA workflow assessment. We'll map your current authorization burden, show you which agents apply to your environment, and model the ROI — before writing a single line of code.
See Agent DemoPrior authorization automation uses AI and intelligent workflows to automatically submit, track, and manage prior authorization requests — eliminating manual back-and-forth with payers and reducing delays in patient care.
By automatically verifying payer requirements, checking eligibility, and submitting complete authorization requests in real time, it significantly reduces incomplete submissions and the denial rates that come with them.
Yes. Our prior authorization automation solutions are built to comply with HIPAA, CMS mandates, and payer-specific guidelines, ensuring every request meets regulatory standards while protecting patient data.
Absolutely. Our solutions integrate seamlessly with your EHR, EMR, and revenue cycle management platforms using HL7 and FHIR APIs, so authorization workflows fit naturally into your existing processes.
The cost depends on the number of payer integrations, workflow complexity, and your existing infrastructure. We assess your specific needs and provide a detailed estimate tailored to your organization's scale and goals.
Implementation typically takes 8 to 16 weeks depending on the number of payer connections, EHR integrations, and specialty workflows involved. We follow a phased rollout — starting with your highest-volume procedures to deliver measurable ROI before full deployment.
Our system automatically detects the denial reason, diagnoses the root cause, and triggers the appeals workflow — generating a clinically accurate reconsideration letter with supporting evidence and re-submitting to the payer, often before your staff is even notified.
Have more questions?
Ask our expertsWe believe knowledge is the key to success journey. And the right knowledge is the key to success. Get the right knowledge by reading our well-researched blogs and staying ahead of the curve.